 Whooping cough, which is also known as pertussis or the hundred day cough, is a described as a highly contagious bacterial infection of the lungs and airways, caused by the Bordetella pertussis bacterium, which infects the lining of the airways – mainly the windpipe (trachea) and the two airways that branch off from it to the lungs (the bronchus/bronchi).
Whooping cough, which is also known as pertussis or the hundred day cough, is a described as a highly contagious bacterial infection of the lungs and airways, caused by the Bordetella pertussis bacterium, which infects the lining of the airways – mainly the windpipe (trachea) and the two airways that branch off from it to the lungs (the bronchus/bronchi).
Onset of symptoms or first stage of infection is usually a persistent dry and irritating cough.
Other symptoms may include:
- runny/blocked nose
- sneezing/watery eyes
- raised temperature
- sore throat
If the bacteria make contact with your airways, this leads to the second stage of infection:
- a build-up of thick mucus – which causes the intense bouts of coughing as your body tries to expel it
- swollen airways – which makes breathing more difficult and causing the “whoop” sound as you gasp for breath after coughing (small children may not make the whooping noise, but appear to be gagging/gasping, temporarily stop breathing)
- vomiting after coughing
- tiredness and redness in the face from the effort of coughing.
Each attack lasts about 1 – 2 minutes – on average 12 – 15 coughing bouts in a day.
People with whooping cough are infectious from six days after exposure to three weeks after the “whooping” cough begins (incubation period). It is thought that the bacteria is passed from person to person by infected droplets in the air (coughing/sneezing).
Conventional treatment of whooping cough
If whooping cough is diagnosed during the first three weeks (21 days) of infection, a course of antibiotics may be prescribed, which is primarily done to prevent the infection being passed on to others (especially to young babies under 6 months of age that are thought to be particularly vulnerable).
When children are admitted to hospital, they may be treated in isolation and antibiotics may be administered intravenously (drip), as well as corticosteroids to help reduce the inflammation/swelling in the lungs (alleviates breathing issues). Extra oxygen may also be given via a facemask, and a bulb syringe used to suction away excess mucous which may be blocking the airways.
The cough is thought to be far less severe in adults and older children. Post 21 days of infection, the GP may be less likely to prescribe antibiotics. Additional advice includes:
- get plenty of rest
- drink lots of fluids to prevent dehydration
- clear away excess mucus or vomit during bouts of coughing so it cannot be inhaled and cause choking
- ibuprofen or paracetamol can be used to relieve other symptoms such as a high temperature and sore throat – aspirin should not be given to children under the age of 16.
Children with whooping cough should be kept away from school or nursery until either:
- five days from the time they start taking antibiotics
- they have had three weeks of intense coughing (unlikely to be infectious after this time).
The same advice applies to adults returning to work.
Recovery stage
Over the period of 2 months or more, fewer and less extreme bouts of coughing will occur.
Homeopathic Treatment of whooping cough
Complementary to any medication you may choose to give / take, please consider the following list of homeopathic remedies to help relieve the symptoms. There may well be other indicated remedies, but these are some of the most commonly used. As mentioned further down in the post, ideally you would have the support of your own homeopath, but I am aware that this may not be available to everyone, and hence my desire to list these remedies for you:


Herbal Support
I am not a qualified herbalist or aromatherapist, but you may like to use herbs or essential oils alongside the homeopathy. Personally I use Neal’s Yard, as they sell loose herbs, have a range of tinctures and most of their essential oils are organic. There will of course be other brands available and your local health food shop is likely to stock a variety of Elderberry products.
A simple and soothing cough remedy suitable for adults and children can be made from a slice of fresh lemon, a teaspoon of honey, and a few drops of Elderberry tincture added to hot water.
Coltsfoot, Elderflower, Sage: Effective selection of expectorant herbs with a soothing and antibacterial action. Make an infusion and drink 3 times a day, or use the tinctures.
Coltsfoot should only be taken for 3-4 days at a time. Do not use coltsfoot or sage during pregnancy or breastfeeding unless prescribed by a qualified practitioner.
Aniseed: Add this for spasmodic or irritating coughs for its antispasmodic action.
Please check whether these are suitable for your child, depending on their age.
Aromatherapy / Essential Oils
Eucalyptus, Frankincense, Thyme Linalol:
inhale the vapours from a bowl of hot water into which two or three drops of each of the essential oils have been added, or dilute in a vegetable base oil to massage onto the chest area.
Please check whether these are suitable for your child, depending on their age.
I also like to use the following WALA product, to rub on the chest and back, but it can be quite expensive unless you can get it on prescription:
WALA Plantago Bronchialbalsam (chest rub)
“Coughing is a useful reflex: it clears the airways. However, when you have a cold, a cough can becomes stubborn and painful and refuse to go away. The medicinal plant extracts and essential oils in WALA’s chest rub Plantago Bronchialbalsam* alleviate coughing fits, dissolve thick mucus and hence facilitate expectoration. When applied to the chest and back this balm forms a gentle, warming shield. It soothes irritated mucous membranes and eases the troublesome urge to cough, without suppressing expectoration. Gentle relief that soon has you breathing freely again.”
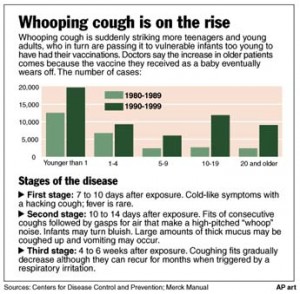
Rise in whooping cough cases
Below is an infographic found online, which, apart from suggesting the vaccinations helped reduce the occurrence of pertussis, claims there is a rise in whooping cough among older patients as immunity is thought to wear off as we grow older.
Whooping Cough Vaccine in Pregnancy
Since October 2012, pregnant women are given the whooping cough vaccine after the 20 week scan, and ideally before 32 weeks, although the NHS website says it can be given up to the point of labour, as it is thought to protect their unborn child during its first few months of life. However, as of 1st April 2016, the vaccine will be offered from 16 weeks onward – “Offering maternal immunisation earlier than the current 28 week recommendation should not only improve infant protection, it will also provide more opportunity for pregnant women to be offered the pertussis vaccine during pregnancy”.
(www.gov.uk/government/uploads/system/uploads/attachment_data/file/510376/PHE_9750_VU_242_March_2016_03_web.pdf)
Some women have questioned the use of the Boostrix IPV/Repevax vaccine during pregnancy as the package insert states that its safety has not been tested on pregnant women. The NHS website says that the benefits of the vaccine outweigh any risks, and that it is standard practice for medicines not to be tested on pregnant women – “This is why the manufacturer’s information leaflet includes this statement, and not because of any specific safety concerns or evidence of harm in pregnancy” – despite this statement claiming there are no safety concerns, the fact remains that they cannot be 100% certain as the vaccines remain untested.
Here is the link to the package insert www.medicines.org.uk/emc/medicine/28679 and an extract from this:
4.6 Fertility, pregnancy and lactation
Fertility
No human data from prospective clinical studies are available. Animal studies do not indicate direct or indirect harmful effects with respect to female fertility (see section 5.3).
Pregnancy
Animal studies do not indicate direct or indirect harmful effects with respect to pregnancy, embryonal/foetal development, parturition or post-natal development (see section 5.3).
As with other inactivated vaccines, it is not expected that vaccination with Boostrix-IPV harms the foetus.
However, human data from prospective clinical studies on the use of Boostrix-IPV during pregnancy are not available. Therefore, Boostrix-IPVshould be used during pregnancy only when clearly needed, and the possible advantages outweigh the possible risks for the foetus. No teratogenic effect of vaccines containing diphtheria or tetanus toxoids, or inactivated poliovirus has been observed following use in pregnant women.
Breastfeeding
The effect of administration of Boostrix-IPV during lactation has not been assessed. Nevertheless, as Boostrix-IPV contains toxoids or inactivated antigens, no risk to the breastfed infant should be expected. The benefits versus the risk of administering Boostrix-IPV to breastfeeding women should carefully be evaluated by the health-care providers.
Here is an extract of the ingredients list for the Boostrix IPV vaccine:
Qualitative and quantitative composition
1 dose (0.5 ml) contains:
| Diphtheria toxoid1 | not less than 2 International Units (IU) (2.5 Lf) |
| Tetanus toxoid1 | not less than 20 International Units (IU) (5 Lf) |
| Bordetella pertussis antigens | |
| Pertussis toxoid1 | 8 micrograms |
| Filamentous Haemagglutinin1 | 8 micrograms |
| Pertactin1 | 2.5 micrograms |
| Inactivated poliovirus | |
| type 1 (Mahoney strain)2 | 40 D-antigen unit |
| type 2 (MEF-1 strain)2 | 8 D-antigen unit |
| type 3 (Saukett strain)2 | 32 D-antigen unit |
| 1adsorbed on aluminium hydroxide, hydrated (Al(OH)3) | 0.3 milligrams Al3+ |
| and aluminium phosphate (AlPO4) | 0.2 milligrams Al3+ |
| 2 propagated in VERO cells |
I tried to find more information on ‘in VERO’ cells and it seems it means they are ‘host cells’ for growing the vaccines – http://au.gsk.com/media/217186/boostrix_ipv_pi_005_approved.pdf
For the Boostrix IPV vaccine the following info is given “The manufacture of this product includes exposure to bovine derived materials” – other vaccines include the use of African Green Monkey cells (influenza vaccine) http://www.ncbi.nlm.nih.gov/pmc/articles/PMC190510/.
Please also be aware that this is NOT a single pertussin vaccine, but that it contains, tetanus, diphtheria and polio (inactivated) as well. On top of this pregnant mums are also offered the flu vaccine, so that makes 5 vaccines in pregnancy.
If you would like some more info here is another link – scroll down through the news items http://www.jayne-donegan.co.uk/news
Whooping Cough Vaccine for Children
Children are vaccinated against whooping cough with the 5-in-1 vaccine at 8, 12 and 16 weeks of age, and again with the 4-in-1 pre-school booster before starting school at the age of about 3 years and 4 months.
I hope this information has been helpful for you. Here is a link to my website www.arnicarocks.co.uk
Useful links:
http://www.nhs.uk/Conditions/Whooping-cough/Pages/Symptoms.aspx
https://www.medicines.org.uk/emc/medicine/28679
http://au.gsk.com/media/217186/boostrix_ipv_pi_005_approved.pdf
https://www.wala.de/english/newsletter/212-02-en/article-3/

Many people actually don’t care about common cough and cold.
Thanks for sharing this wonderful information with us.